Biologically Active Form of B12
5000 mcg
60 Lozenges ( SKU: 9422U )
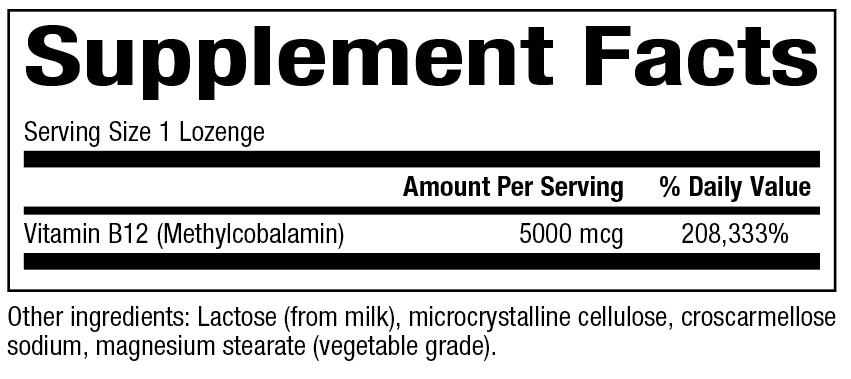
Supplement Facts:

Dosage:
Suggested Usage: Chew and swallow 1 lozenge per day or as directed by a health care professional.
Allergens:
Contains no artificial colors, preservatives, or sweeteners; no starch, sugar, wheat, gluten, yeast, soy, corn, egg, fish, shellfish, salt, tree nuts, or GMOs. Suitable for vegetarians.
